Dental Risk Factors Associated with Diabetes
Diabetes affects more than just blood sugar—it impacts your entire body, including your oral health. People with diabetes face a higher risk of dental problems due to blood sugar fluctuations. These create an ideal environment for bacteria to thrive. By understanding the dental risk factors associated with diabetes and taking preventive measures, you can protect your smile and avoid complications.
Increased Risk of Gum Disease
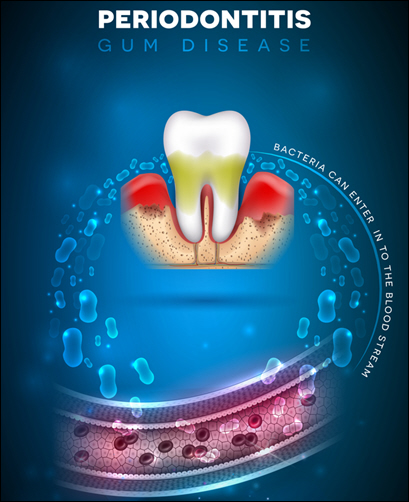 Gum disease, or periodontal disease, is one of the most common oral health concerns for people with diabetes. High blood sugar levels allow harmful bacteria to grow, which can lead to plaque buildup along the gumline. If left unchecked, plaque irritates the gums, causing redness, swelling, and bleeding—early signs of gingivitis. Over time, this can progress to periodontitis, a more severe form of gum disease. Periodontitis damages the gums and supporting bone structure, increasing the risk of tooth loss.
Gum disease, or periodontal disease, is one of the most common oral health concerns for people with diabetes. High blood sugar levels allow harmful bacteria to grow, which can lead to plaque buildup along the gumline. If left unchecked, plaque irritates the gums, causing redness, swelling, and bleeding—early signs of gingivitis. Over time, this can progress to periodontitis, a more severe form of gum disease. Periodontitis damages the gums and supporting bone structure, increasing the risk of tooth loss.
Poorly managed diabetes can make it harder for your body to fight off infections, making it easier for gum disease to develop and worsen. Regular dental check-ups and consistent at-home care can help manage this risk.
Dry Mouth and Decay
People with diabetes often experience dry mouth, a condition where saliva production decreases, leaving the mouth dry. Saliva plays a crucial role in washing away food particles and bacteria that cause decay. Without enough saliva, your mouth becomes more acidic, creating an environment where bacteria can thrive, leading to increased cavities and discomfort.
Dry mouth also leads to irritation and sores, which can make eating and speaking uncomfortable. Staying hydrated and using saliva substitutes can help manage dry mouth and reduce the risk of tooth decay.
Delayed Healing and Higher Infection Risk
 Diabetes slows down the body’s natural healing process, which can complicate dental procedures. Even minor injuries, like a small sore on the gums or a tooth extraction site, may take longer to heal, increasing the chance of infection. This delayed healing can also make it more challenging to manage oral health issues like gum disease or ulcers. Dentists may take extra precautions when treating patients with diabetes to reduce the risk of post-procedure infections.
Diabetes slows down the body’s natural healing process, which can complicate dental procedures. Even minor injuries, like a small sore on the gums or a tooth extraction site, may take longer to heal, increasing the chance of infection. This delayed healing can also make it more challenging to manage oral health issues like gum disease or ulcers. Dentists may take extra precautions when treating patients with diabetes to reduce the risk of post-procedure infections.
Thrush and Other Fungal Infections
People with diabetes are more susceptible to fungal infections, like thrush, which is caused by an overgrowth of Candida, a naturally occurring yeast. High blood sugar levels create a favorable environment for yeast, especially in a dry mouth. Thrush causes white or red patches on the tongue, inner cheeks, and gums, leading to soreness and discomfort. Practicing good oral hygiene and managing blood sugar can help lower the risk of developing these infections.
Taking Steps to Protect Your Oral Health
Fortunately, with proper management, you can minimize these risks and maintain good oral health. Here’s how:
- Maintain Blood Sugar Levels: Keeping blood sugar levels within your target range reduces bacterial growth, supporting gum health and reducing dry mouth symptoms.
- Practice Consistent Oral Hygiene: Brushing twice daily, flossing, and rinsing with an antibacterial mouthwash removes plaque and bacteria, keeping your gums healthy.
- Visit Your Dentist Regularly: Regular check-ups allow your dentist to monitor for early signs of gum disease or other concerns, so they can be addressed quickly. Let your dentist know if you have diabetes, as they can tailor care to fit your needs.
By taking these proactive steps, you can manage your oral health and avoid complications related to diabetes, keeping your smile healthy and your overall wellness intact.


